At 3:15 on a winter morning, the underground haul road sits at its quietest and its most dangerous. Low-lux emergency lighting throws cold pools onto the ribs, a 90-tonne truck cycles past the tip at the bottom of the decline, and in the surface control room the only sound is the slow tick of the ventilation fans. This is the circadian trough — the two-to-six window when core body temperature bottoms out, reaction times slow, and the brain will take microsleeps whether the operator consents or not. Behind the console, the night-shift dispatcher is on hour sixteen of a fourteen-day rotation.
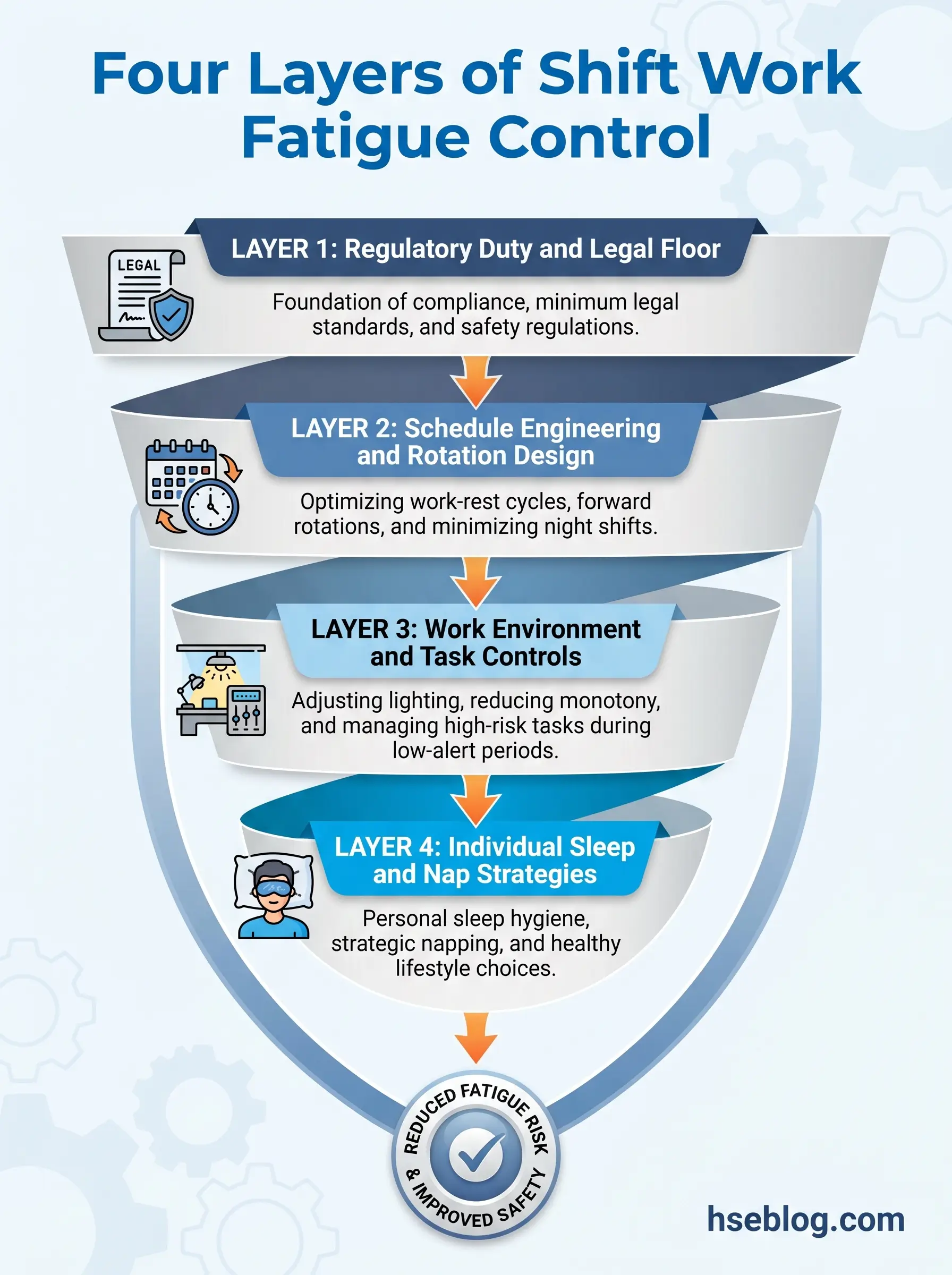
Roughly a quarter of the workforce in industrialised economies — more than 3.5 million people in the UK alone — works non-standard hours, and fatigue has been implicated in the major process-safety disasters of the last forty years, from Texas City to Chernobyl to Exxon Valdez. For decades it was treated as a personality flaw, not a systems-level hazard. That framing has shifted. Managing fatigue in shift workers is now an employer duty under ISO 45001, HSE HSG256, and the OSHA General Duty Clause — and this guide walks through best practices across four layers: regulatory duty, schedule engineering, the work environment, and individual support.
What Is Fatigue in the Shift Work Context?
Occupational fatigue is not simply being tired. It is a decline in mental and physical performance produced by three drivers acting together: sleep homeostasis (how long you have been awake and how much sleep debt has built up), circadian rhythm (where you sit in the 24-hour body clock), and workload (the duration and intensity of the task). A night-shift operator on day four of a rotation might arrive at the gate having slept only four hours in a warm bedroom, work the circadian low point at 3 AM, and then drive home when her reaction time is at its worst. HSG256 defines fatigue as the decline in mental or physical performance that results from prolonged exertion, sleep loss, and disruption of the internal clock.
One distinction most awareness training gets wrong: sleepiness is not the same as fatigue. I brief new supervisors on this every induction, because it changes how they read the people in front of them.
| Dimension | Sleepiness | Fatigue |
|---|---|---|
| Core feeling | Drive to fall asleep | Exhaustion, reduced capacity |
| Relieved by | Sleep | Rest, recovery, and load reduction |
| Main driver | Sleep debt plus circadian phase | Sleep loss, prolonged exertion, mental load |
| Hidden risk | Micro-sleeps at the wheel or console | Errors, slowed judgement, mood shifts |
Acute fatigue builds across a single long shift and clears with one good sleep. Cumulative fatigue builds across weeks of compressed rosters and broken sleep, and it does not clear on a single day off. Sleep debt is real, measurable, and cumulative — and the 2:00 to 6:00 AM window is when the combined biological dip is deepest.
The True Cost: Health and Safety Risks of Shift Worker Fatigue
The published evidence is blunt. Injury rates run 18% higher on evening shifts and 30% higher on night shifts compared with day shifts. Working 12-hour days is linked to a 37% increase in injury risk. NIOSH’s own analysis puts accident and error risk up 28% on nights and 15% on evenings relative to a day-shift baseline.
Worker health effects are equally documented. Cardiovascular and metabolic disease risk climbs with years of rotating nights — including stroke and ischaemic heart disease at weekly hours above 55, per WHO and ILO joint estimates. The International Agency for Research on Cancer classifies night-shift work that disrupts circadian rhythms as “probably carcinogenic” (Group 2A). Shift Work Disorder — insomnia and excessive sleepiness tied directly to shift timing — affects around 14% of night and 8% of rotating-shift workers in large US samples, with some studies placing the broader prevalence around 27%.
On the operational side, fatigue sits behind a disproportionate share of serious incidents. The UK’s HSE estimates fatigue is implicated in around 20% of major-road accidents and costs the UK economy £115 to £240 million a year in workplace incidents alone. The 2005 Texas City refinery explosion, which killed fifteen workers, drove API to issue RP 755 — a sector-specific fatigue standard born directly from that investigation.
Spotting the Warning Signs Early
Supervisors who can spot fatigue early stop incidents before they reach the sharp end. Most training reduces the signs to “yawning and rubbing eyes” and stops there. The signals actually sit across three layers.
Physical signs on the shift floor:
- Micro-sleeps and head nods — the two-to-ten-second lapses with eyes open that precede full sleep.
- Slowed hand–eye coordination — fumbled radio clicks, missed handholds, late gear changes on mobile equipment.
- Repeated yawning, eye rubbing, heavy blinking — especially clustered between 2 and 6 AM.
- Poor posture and slumping in the cab or at the console.
Cognitive signs a supervisor should be trained to read:
- Memory lapses — forgetting steps in a lock-out, repeating radio calls, losing place in a checklist.
- Slowed reaction time — measurable by psychomotor vigilance tests, visible as late responses to alarms.
- Tunnel thinking — fixation on one instrument or one task while others drift.
- Poor risk judgement — a crew that normally stops work pushes through instead.
Behavioural and organisational signals that show up in the data:
- Incidents and near-misses clustering in a specific time window, typically 2–6 AM and 14:00–16:00.
- Rising absenteeism and late arrivals at a particular point in the rotation.
- Shift-swap requests spiking — often a proxy for fatigue from quick-returns.
- Mood shifts — irritability, flat affect, and withdrawal from toolbox talks.
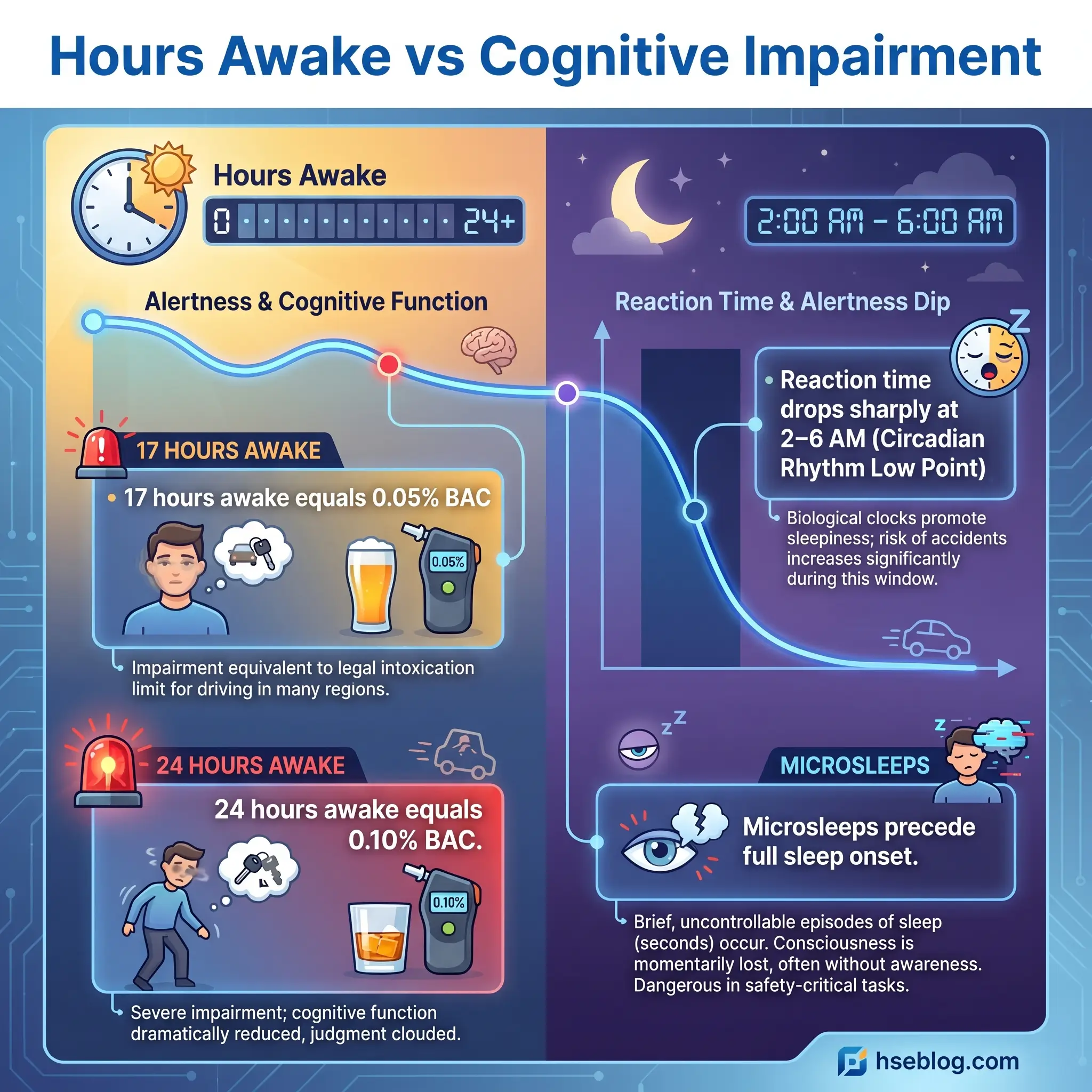
A calibration point every supervisor should carry: being awake for 17 hours produces cognitive impairment roughly equivalent to a blood alcohol content of 0.05%. Nobody on our site would hand a haul-truck key to someone at 0.05%. A worker 17 hours into a bad rotation is operationally indistinguishable.
Best Practice #1: Design Shift Schedules for Human Biology
HSE HSG256 is explicit on this point: shift schedule design is the single most powerful control because it eliminates or reduces fatigue at the source. Engineering the roster sits above anything you can do with lighting, caffeine, or willpower.
Drawing on the Working Time Society consensus (Wong et al., 2019), ACOEM’s 2012 guidance, and HSG256, a defensible shift design applies these principles:
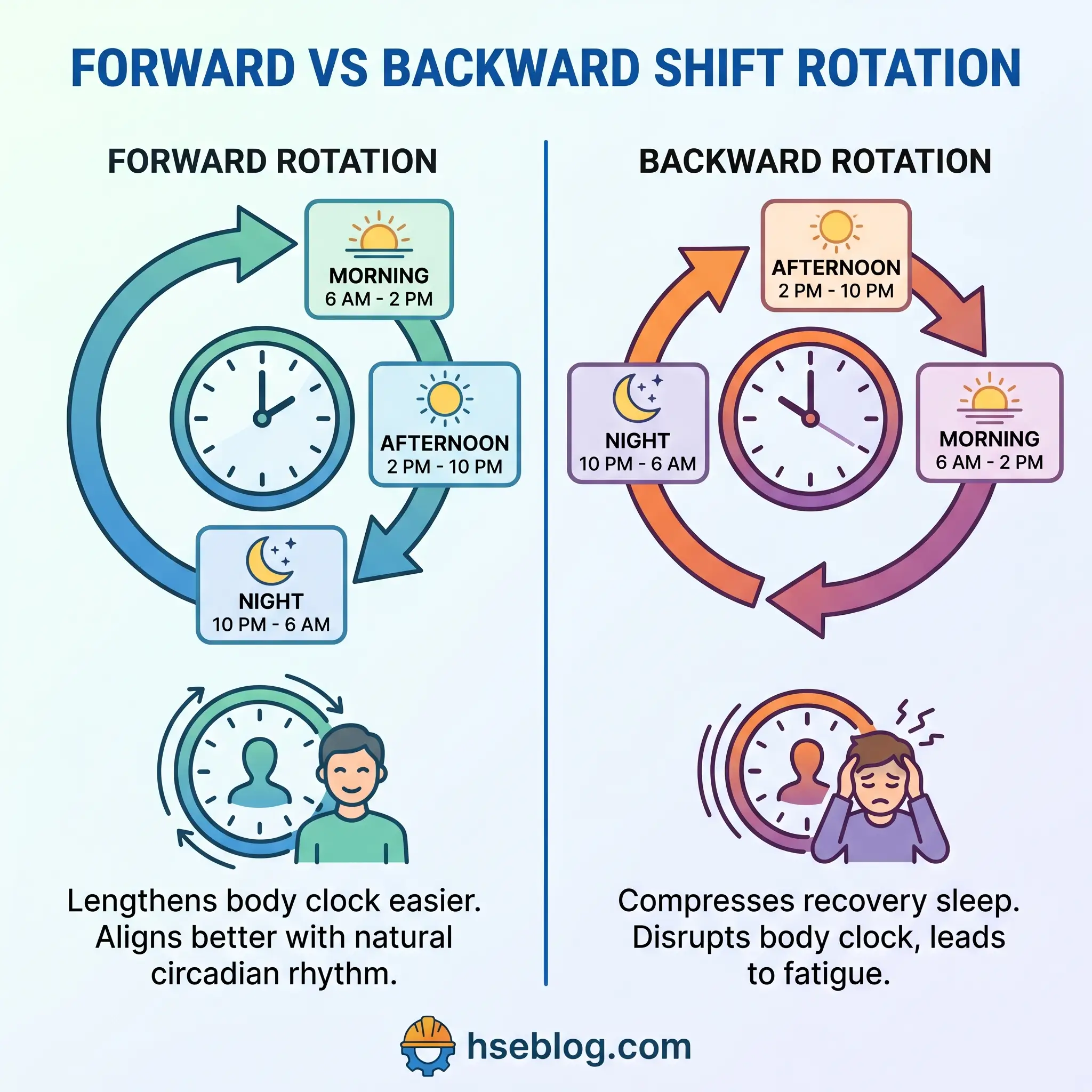
- Rotate forward, not backward. Morning → afternoon → night is easier for the circadian clock to accommodate than a reverse cycle. The internal clock lengthens more naturally than it shortens.
- Cap consecutive night shifts at three where operationally feasible. The absolute ceiling, even under relaxed rosters, is five to seven consecutive shifts of any type.
- Guarantee a minimum 11-hour inter-shift rest. Quick-returns — a late shift followed by an early shift — compress sleep and are one of the most fatiguing patterns the literature identifies.
- Keep safety-critical shifts at 8 hours where possible. Where 12-hour shifts are operationally locked in, restrict overtime aggressively and rotate demanding tasks within the shift.
- Build a 48-hour break after every night-shift block. A single day off is not enough to clear a night-block sleep debt.
- Risk-assess overtime, on-call, and shift-swaps. Swap approvals should check cumulative hours, rest opportunity, and cumulative fatigue load — not just headcount.
On our haulage fleet, a switch from a traditional 7-on/7-off backward rotation to a 4-on/4-off forward-rotating pattern with three-night maximums materially reduced 2–6 AM incidents over the following two rotations. Compliance with the UK Working Time Regulations and the EU Working Time Directive is a baseline. HSE’s fatigue guidance states it plainly — statutory hour limits alone do not discharge the employer’s duty.
Using Fatigue Risk Assessment Tools
Rosters should be quantitatively tested before deployment. Biomathematical models — FAID, SAFTE-FAST, and the HSE Fatigue and Risk Index — score a proposed schedule for expected fatigue load based on shift timing, duration, rest opportunity, and cumulative exposure. They do not replace field judgement, but they catch combinations of overtime and shift-swap that look fine on paper and score red when modelled.
Best Practice #2: Build a Fatigue Risk Management System (FRMS)
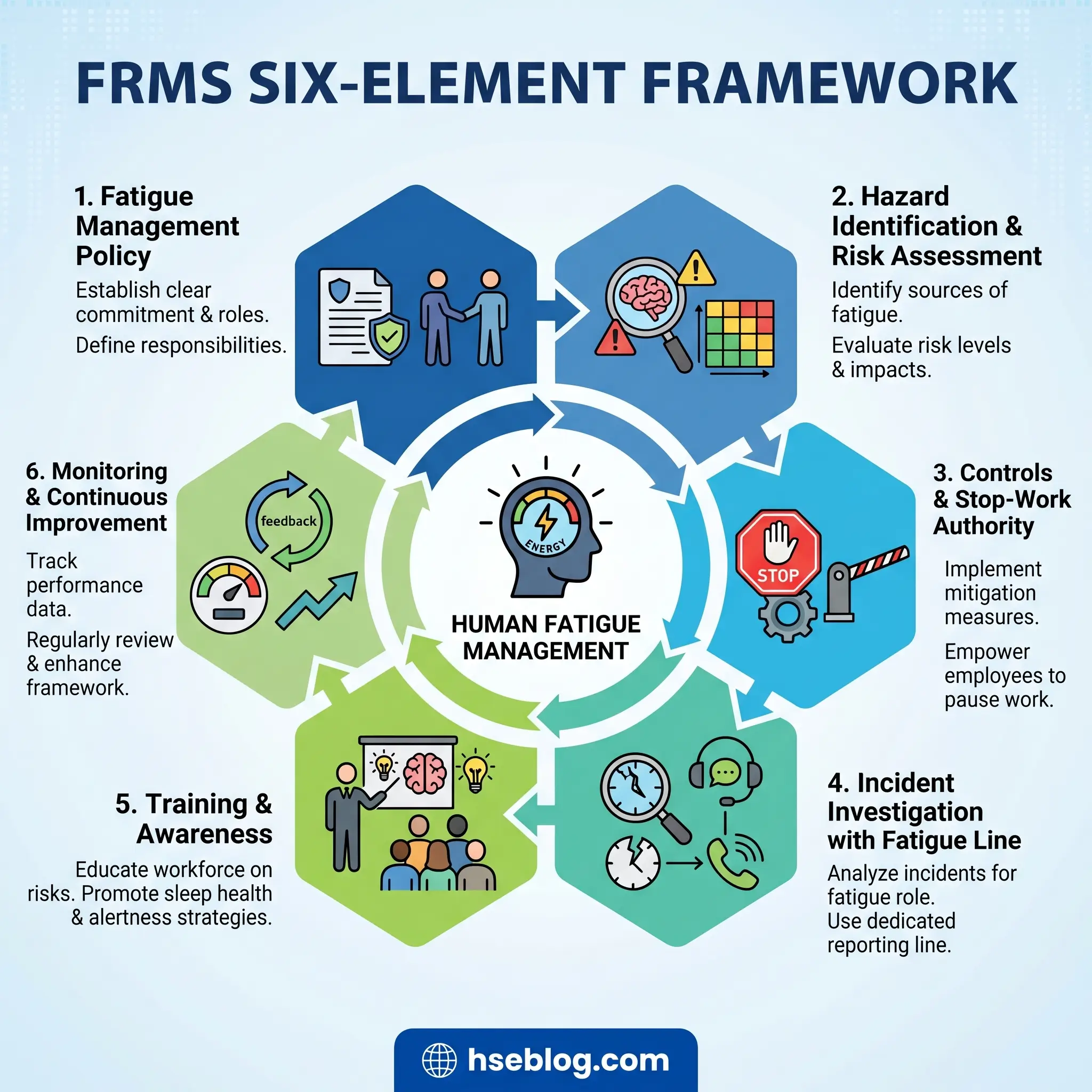
An FRMS is the governance layer that sits on top of schedule design. It is what turns a rostering spreadsheet into a managed-hazard program defensible under ISO 45001 Clause 6.1. Drawing on ACOEM’s 2012 guidance, ICAO’s FRMS framework, and NIOSH’s work-schedules resources, six elements form the backbone.
- Fatigue management policy — a signed, senior-leader-owned document that names fatigue as a hazard, assigns accountability, and sets out rules on maximum hours, rest, and reporting.
- Hazard identification and risk assessment — mapping high-risk hours, tasks, and roles, and scoring rosters with biomathematical tools before deployment.
- Controls — scheduling rules, staffing levels, task rotation within shifts, and explicit stop-work authority when a worker or supervisor declares a fatigue hazard.
- Incident investigation — every investigation must explicitly test whether fatigue was a contributor, through a standard question set rather than an optional checkbox.
- Training and awareness — layered by audience: workers, supervisors, and managers each get different content.
- Performance monitoring and continuous improvement — objective data (overtime hours, time-of-day incident distribution) plus subjective tools such as the Karolinska Sleepiness Scale, fed through a PDCA loop aligned with ISO 45001 Clause 10.
Watch For: Near-misses that cluster between 2 and 6 AM are your most sensitive fatigue indicator. If your incident system does not break down reports by hour of day, you are blind to your highest-risk window.
A FRMS that lives only in a binder is an audit trophy, not a risk control. The one element that makes the rest work is a no-blame reporting culture — workers have to be able to declare “unfit for duty” without losing a shift’s pay or their supervisor’s trust. I have watched two sites implement identical FRMS documents with opposite outcomes; the difference was always whether leadership backed the first worker who called themselves out.
Best Practice #3: Optimize the Work Environment for Alertness
Environmental controls do not replace schedule design, but they can shift alertness measurably on the shift itself. Every one has a biological mechanism you can trace.
- Bright, blue-enriched lighting at 500 lux or higher in the first half of the night shift suppresses melatonin and lifts alertness. Task areas should be lit like a daytime workplace, not a mood-lit office.
- Warmer, dimmer lighting in the last two hours of the night shift to allow the melatonin curve to start recovering before the commute home.
- Cool ambient temperatures (roughly 19–21°C) support alertness. Overheated control rooms are notorious sleep-room equivalents.
- Designated quiet rest and nap rooms — cool (16–20°C), dark, private, with booking procedures. Couches in the mess room do not qualify.
- Task rotation to keep the most monotonous or safety-critical tasks out of the 2–6 AM window where circadian troughs are deepest.
- Access to protein-forward food and water through the night — vending-only nutrition is correlated with metabolic morbidity in longitudinal shift studies.
The easiest diagnostic: walk your own night shift at 3 AM and look at the lighting on the task at hand, not at the ceiling. Most “well-lit” facilities fail at the work plane.
Best Practice #4: Strategic Napping and Rest Breaks
Napping has the strongest evidence base of any individual-level fatigue control, yet in most industries it is either forbidden or mismanaged. Both approaches create risk. Forbidding naps wastes a cheap, well-evidenced countermeasure; allowing naps without policy creates sleep-inertia accidents.
A defensible approach gives precise guidance on duration, timing, and post-nap recovery.
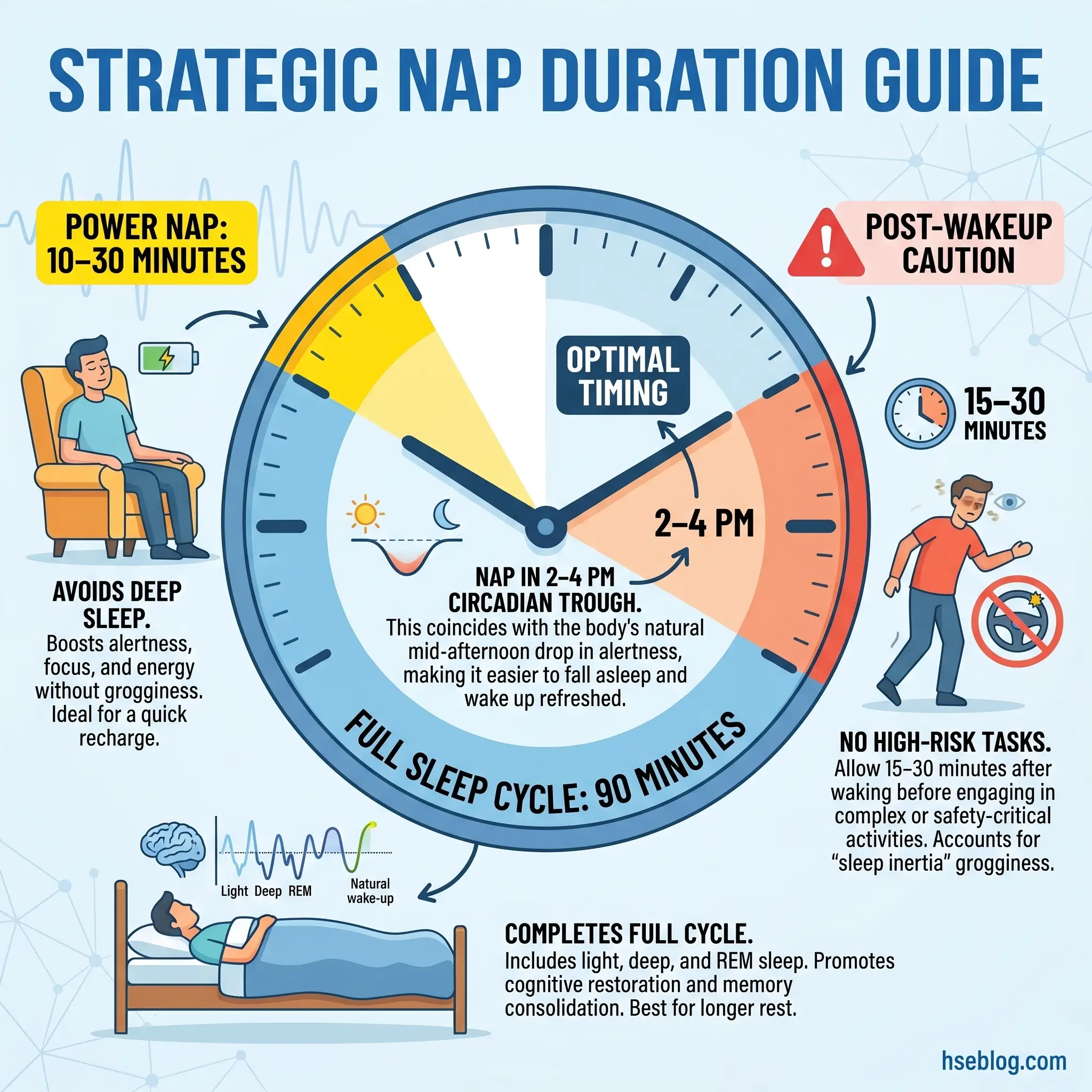
- Pre-shift nap: Ideally a full 90-minute sleep cycle before a night shift. If only 20–30 minutes is available, take it — short naps still deliver measurable alertness gains.
- On-shift nap: Keep it between 10 and 30 minutes. Longer naps risk entering slow-wave sleep, which produces severe sleep inertia on waking.
- Timing: Place the nap within the circadian trough, roughly 2:00–4:00 AM. That is when the alertness return-on-time-invested peaks.
- The caffeine nap: Take about 200 mg of caffeine immediately before a 15–20 minute nap. Caffeine reaches peak plasma concentration at 20–30 minutes, so the worker wakes to both natural recovery and caffeine onset.
- Sleep inertia: The 15–30 minutes (sometimes up to two hours) of impaired performance after waking. Policy should prohibit driving, operating mobile plant, or starting any safety-critical task during the inertia window.
- Written policy and dedicated facilities: Napping works when it is sanctioned, logged, and physically supported — not when a worker hides behind an MCC panel.
The Fix That Works: Pair a 20-minute nap with a scheduled supervisor callback 15 minutes after the alarm. It normalises napping, catches anyone who slept longer than planned, and flushes out sleep inertia before the worker returns to a high-risk task.
Best Practice #5: Support Sleep Hygiene Tailored to Shift Workers
Generic sleep hygiene advice — “no naps during the day”, “sleep at the same time every night” — is wrong for shift workers. Much of it actively contradicts the reality of a rotating roster. The Shriane et al. 2023 Delphi-consensus guidelines, the first expert framework designed specifically for shift workers, replace the day-worker orthodoxy with something shift-specific.
Sleep environment:
- Complete darkness — blackout blinds, a quality eye mask, door blinds blocking hallway light.
- Cool (16–20°C) and quiet — white-noise machine, earplugs, separate room from household traffic where possible.
- Phone and pager on a silent routing tree — only designated call-back contacts should break sleep.
Substances and timing:
- Caffeine timed to the shift, not the clock — moderate doses early; cut-off 3–4 hours before intended sleep (longer cut-offs of 8–10 hours are safer for sensitive sleepers).
- Alcohol as a sleep aid is a trap — it fragments the second half of sleep and reduces recovery value.
- Melatonin only under medical guidance — effective for circadian shifting when timed correctly, ineffective or counter-productive otherwise.
Routine and load:
- Protect 7–9 hours of sleep per 24 hours, even when split into an anchor sleep plus a pre-shift nap.
- Wind-down protocol on the commute home — sunglasses to reduce bright-light exposure, no screens for the last hour before sleep.
- Light, protein-forward meals finished 2–3 hours before intended sleep.
Individual factors:
- Chronotype-matched scheduling where operationally possible. Confirmed evening types (“night owls”) tolerate nights better than confirmed morning types. Self-report tools such as the Munich Chronotype Questionnaire can inform voluntary shift-preference systems.

Best Practice #6: Train Supervisors and Workers
Training is a required pillar under ISO 45001, HSE HSG256, OSHA’s General Duty Clause, and the ACOEM framework. A credible FRMS trains three audiences with different content.
Workers need to understand how fatigue is caused, how it presents, and how cumulative sleep debt works. They need shift-specific sleep hygiene and strategic napping technique, their personal duty to arrive fit for duty, and the no-blame route to declare “unfit for duty.”
Supervisors need to be trained to recognise fatigue impairment in real time across physical, cognitive, and behavioural cues. They need to conduct a fit-for-duty conversation without defaulting to discipline, reassign or stand a worker down when necessary and document the decision, and apply stop-work authority when fatigue risk is present.
Managers and leaders need to understand FRMS governance, biomathematical roster scoring, and PDCA integration with the OH&S management system. They need fluency in their legal duties under local regulation and ISO 45001 — and a hard look at how their own rhetoric, praising “heroes” who pull triple shifts, undermines the program.
A colleague running a refinery turnaround told me he spent more time training the general foremen on fatigue conversations than on any other safety topic during the shutdown. His incident-free turnaround made the case.
Best Practice #7: Use Monitoring Technology Wisely
The last five years have produced a genuine market for fatigue-monitoring technology. Used well, it augments schedule design and FRMS governance. Used badly, it becomes a surveillance tool that undermines the no-blame reporting culture the FRMS depends on.
Tool categories currently deployed across 24/7 industries:
- Biomathematical fatigue models such as FAID, SAFTE-FAST, and the HSE Fatigue and Risk Index, scoring rosters before and during deployment.
- Wearables — ring and wrist devices tracking sleep duration, efficiency, and timing, producing individualised fatigue scores.
- In-cab and in-vehicle monitoring using eye-tracking, PERCLOS, lane-deviation, and steering input; widely deployed in haulage, rail, and long-haul trucking.
- Psychomotor Vigilance Task (PVT) devices — a three-to-five-minute reaction-time test validated against sleep deprivation, used for fit-for-duty checks in safety-critical roles.
A 2024–2026 trend worth noting: the move from reactive detection — cameras that alarm when a driver is already nodding — to proactive prediction, where biomathematical models combined with wearable data forecast individualised fatigue 24–30 days ahead of a scheduled shift. The NIOSH fatigue resources flag this maturation, and several mining and logistics operators have deployed variants.
Audit Point: Ask who owns the wearable data, what the retention period is, whether workers can opt out without penalty, and whether fatigue data has ever been used in a disciplinary hearing. If the answers are not clear, the system will erode trust before it delivers value.
Technology is augmentation, not substitution. A site with an exhausting roster and a dashboard of fatigue scores is still an exhausted site.
Legal and Regulatory Duties You Must Meet
Fatigue management sits inside a mature international regulatory framework. The anchors that matter across jurisdictions:
- ISO 45001:2018 — Clauses 6.1 (hazard identification and risk assessment) and 5.4 (worker consultation and participation) require fatigue to be identified as an OH&S hazard, controlled through the management system, and improved continually. A documented FRMS is the most defensible way to demonstrate Clause 6.1 compliance for shift operations.
- HSE (UK) HSG256 — Managing Shift Work — establishes the employer’s legal duty under the Health and Safety at Work Act to assess and manage shift-work fatigue; requires a written fatigue policy addressing hours, overtime, and shift-swapping.
- UK Working Time Regulations 1998 / EU Working Time Directive (2003/88/EC) — minimum 11 consecutive hours rest per 24, 24-hour break per seven days, 48-hour average weekly working cap, and a health assessment for night workers. HSE is clear that compliance alone is not sufficient to control fatigue risk.
- OSHA General Duty Clause, Section 5(a)(1) of the OSH Act 1970 — used to require a workplace free from recognised hazards; fatigue meets the recognised-hazard threshold where extended or irregular shifts create serious risk. The OSHA worker-fatigue prevention guidance supports enforcement.
- ACOEM 2012 Fatigue Risk Management Guidance Statement — the canonical multi-component FRMS framework adopted across industries.
- ILO / Working Time Society Consensus Statements (Wong et al., 2019) — multi-level recommendations on forward rotation, 11-hour inter-shift rest, consecutive-shift caps, and combined prescriptive-plus-risk-based controls.
- Sector-specific standards — API RP 755 (refining and petroleum, post-Texas City), ICAO FRMS (aviation), and hours-of-service regulations in road and rail transport.
Industry-Specific Considerations
Best practices translate across industries, but the pinch-points differ. Healthcare runs into 12-hour nursing shifts that compress sleep and compound with residents’ extended duty periods, and patient-safety errors cluster late in the shift. Transport and logistics live under hours-of-service rules that provide only the floor; the real work is scheduling depot starts out of the 2–6 AM window and deploying in-cab monitoring without creating a punitive data culture. Oil, gas, and mining stack schedule fatigue on top of long commutes or fly-in/fly-out rosters of 14-on/14-off or longer, and API RP 755 applies to refining. Manufacturing and continuous process industries face machine-paced monotony in the circadian trough, where task rotation and alertness monitoring matter more than in non-continuous operations. Emergency services operate under unpredictable demand, cumulative sleep debt across multi-incident shifts, and a culture of heroism that actively resists fatigue reporting.
Building a Fatigue-Aware Culture
Policies, schedules, and technology all fail without the cultural layer. Workers will not declare themselves unfit if doing so costs them a shift’s pay, their supervisor’s approval, or their next promotion.
A fatigue-aware culture shows up in specific, observable ways. Leaders visibly take their own rest and do not celebrate “hero” overtime. Fatigue reports are decoupled from performance management and discipline. Every incident and near-miss investigation includes a fatigue line of inquiry by default. Workers are included in schedule design through self-scheduling pilots where operationally feasible. And fatigue metrics — hours worked, overtime proportion, time-of-day incident distribution — sit alongside productivity on leadership KPI dashboards. The single most powerful cultural signal I have seen was a site general manager standing a foreman down for a shift after a poor sleep the night before, publicly and without penalty. The next month’s fatigue-reporting rate tripled.

Frequently Asked Questions
Conclusion: Treating Fatigue as a Managed Hazard
Managing fatigue in shift workers is not a single intervention. It is the disciplined combination of four layers — engineered schedules that work with circadian biology, an FRMS that governs and monitors the system, a work environment that supports alertness, and individual sleep and nap strategies backed by the organisation. Each layer without the others fails in predictable ways: a good roster with a punitive culture will not be declared against; a perfect FRMS document without supervisor training is a binder.
The test for any operation running shifts is simple. Pull your last twelve months of incidents and near-misses and break them down by hour of day. If you cannot produce that chart in under an hour, your fatigue hazard is not being monitored. If you can produce it and the 2–6 AM cluster is there, your controls are not working. Move beyond the floor set by the Working Time Regulations, commit to the full framework, and treat fatigue with the same discipline the industry already applies to every other recognised hazard.

